
Fundraising
Help Us Raise
Epilepsy Awareness
Become a Volunteer

Epilepsy is still the most common, serious neurological condition in the world but it impacts each person’s life in a unique and individual way.
From May 23 to May 29, National Epilepsy Week will be taking place to raise awareness for those affected by epilepsy, what epilepsy is, who’s affected and what can be done to help those who suffer from this condition.
19th May to 26th May 2026
NATIONAL EPILEPSY WEEK
Epilepsy
Table of contents
Help spread epilepsy awareness
What is epilepsy?
How common is epilepsy?
There are
people
suffering from epilepsy in the UK
Why does it matter?
- 1 in 100 will have a Seizure in their Lifetime
- 40 Types of Epilepsy (Click here for free PDF)
- In the West Midlands 53,000 suffer from Epilepsy
- Epilepsy is the 4th Most Common Neurological Condition
- There are 600,000 People Suffering from Epilepsy in the UK
- Around the World an Estimated 65 Million People have Epilepsy at any given time
- Approximately 1 in 26 people will develop epilepsy at some point in their lifetime
How Epilepsy Affects Lives
Types of seizures
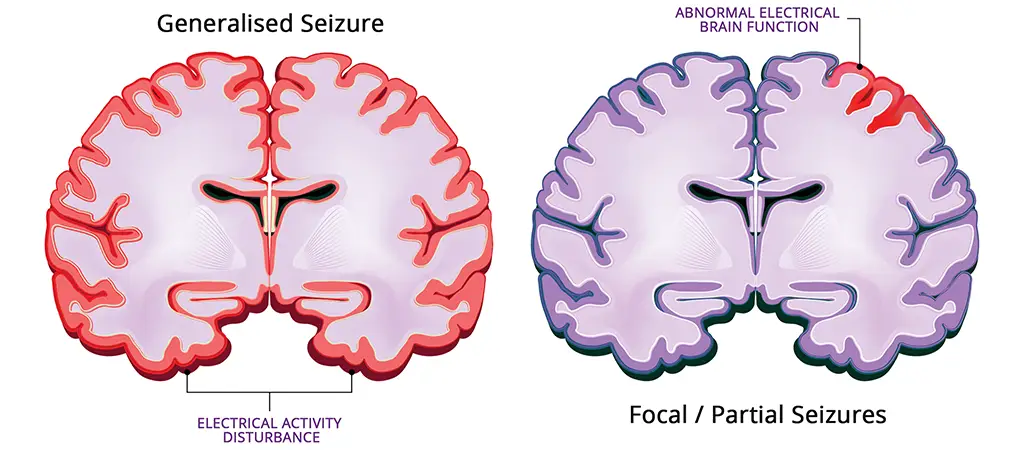
Generalised seizures
- Tonic clonic – Muscle stiffening (tonic stage) and fall to the ground, followed by jerking/convulsive movements (clonic stage). Can last several minutes (previously known as ‘grand-mal seizures’).
- Tonic – Muscle stiffening, fall to the ground.
- Atonic – Loss of muscle tone, fall to the ground. Recovery usually swift.
- Myoclonic – Muscle jerks. Loss of consciousness is usually so brief it is hardly noticeable.
- Absence – Often mistaken for day dreaming. Person goes into brief trance-like state (previously known as petit-mal seizures).
Focal / partial seizures
- Simple focal seizure – Doctors also refer to simple focal seizures as focal aware seizures.
- During a simple focal seizure, a person remains conscious throughout the event and remembers it when it is over. The episode lasts less than a minute.
- Complex partial seizure – Doctors also refer to complex partial seizures as focal impaired awareness seizures.
- When a person has a complex partial seizure, they lose consciousness during the episode and do not remember the seizure after it is over. The seizure may last for more than a minute.
Common symptoms of seizures
- Confusion
- Wandering
- Jerks & twitches
- Shaking or falling
- Picking or lip smacking
- Staring & unresponsiveness
- Whole body convulsions – grand mal seizure
How is epilepsy treated?
Medication
- Your type of epilepsy
- Your age
- Other medicines that you may take for other conditions
- Possible side effects
- Whether you are pregnant or planning a pregnancy
Surgery
Multiple Subpial Transections

Resective Surgery
Temporal Lobotomy
- Removal of a portion of the temporal lobe of the brain
- It is the most common type of epilepsy surgery
- After surgery, 60% to 70% of patients are seizure free
- Removal of a portion of the frontal lobe
- It is the second most common type of epilepsy surgery
- After temporal lobotomy 30% to 50% of patients are free of seizures that impair consciousness or cause abnormal movements
Hemispherectomy
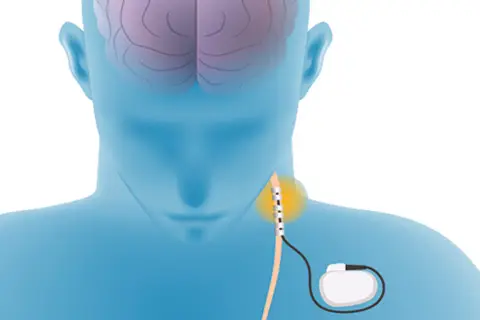
Vagus Nerve Stimulation (VNS)
– A treatment for epilepsy where a small generator is implanted under the skin below the left collarbone. The vagus nerve is stimulated to reduce the frequency and intensity of seizures. This can be suitable for some people with seizures that are difficult to control with medication. The ketogenic diet is a diet very high in fat, low in protein and almost carbohydrate-free. This can be effective in the treatment of difficult-to-control seizures in some children.
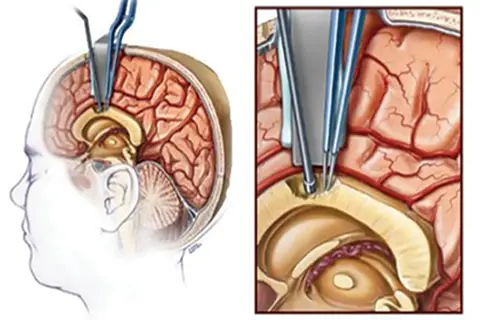
Corpus – Colostomy
Ketogenic diet
- The name ketogenic means that it produces ketones in the body. (keto = ketone; genic = producing) Ketones are formed when the body uses fat for its source of energy.
- Usually the body uses carbohydrates (such as sugar, bread, pasta) for its fuel. Because the ketogenic diet is very low in carbohydrates, fats become the primary fuel instead. The body can work very well on ketones (and fats).
