If you have seizures which can’t be controlled with epilepsy medicines, and you are not able to have epilepsy brain surgery, then vagus nerve stimulation (VNS) therapy may be an option for you. The aim of VNS therapy is to reduce the number of seizures you have and make them less severe.
VNS therapy involves having a small device, called a generator, implanted under the skin of your chest. The generator sends electrical pulses to your brain through a lead attached to a nerve in your neck called the vagus nerve.
How does vagus nerve stimulation therapy work?
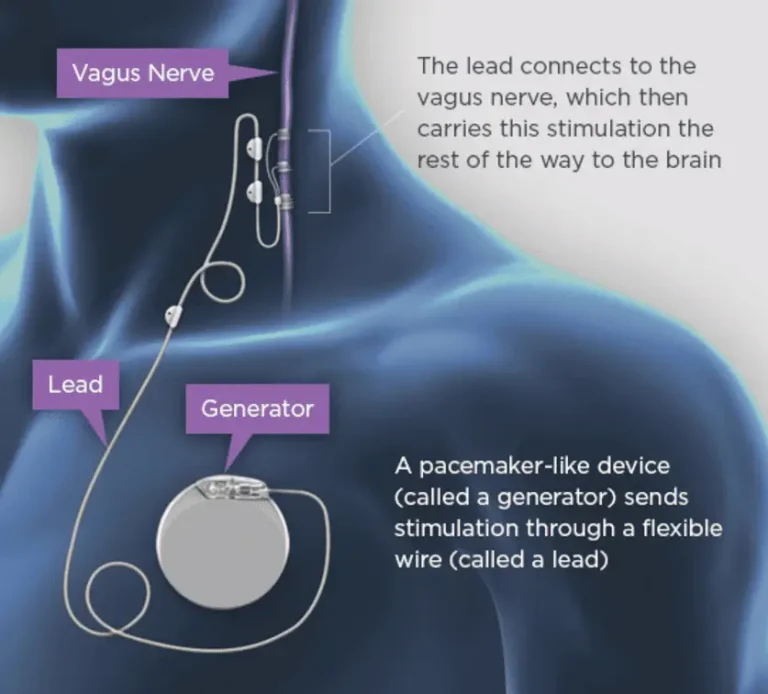
The VNS system is made up of 3 parts:
- A small pacemaker-like device, called a generator
- A thin, flexible wire, called a lead
- A hand-held magnet
The vagus nerve sends messages between the brain and other parts of the body. In VNS therapy the generator is individually programmed to send electrical pulses to the vagus nerve at regular intervals, all day, every day. These pulses are then carried by the vagus nerve to the brain. This regular stimulation can help to reduce the number of seizures you have and make them less severe.
You can also sweep the hand-held magnet over the generator to send an extra dose of therapy to the vagus nerve. This could be if you feel a seizure starting, or when you are having a seizure. This can stop a seizure happening, shorten the seizure or make the seizure less severe. A carer, or family member, can also use the magnet if they see you having a seizure.
The Auto-Stimulation Feature
Many people will be implanted with a VNS with an auto-stimulation feature. With auto stimulation the device will give an extra stimulation when the heart rate reaches a certain level quickly. This quick increase in the heart rate may mean the person is starting to have a seizure, and this extra stimulation may stop or shorten the seizure.
How is it inserted?
To have a VNS put in place, you will need an operation by a paediatric neurosurgical team. You will be asleep under general anaesthetic, through out the procedure.
During the operation a small opening will be made to the left side of the chest where the medical device will be placed inside. Another small opening will be made for the wires to be attached to the vagus nerve. The wire travels under the skin up the left side of the neck and is connected to both the medical device and the vagus nerve.
The wounds will be closed with dissolvable stitches. Pain relief will be given to you during the operation.
What happens after the operation?
After the operation and once awake, you will be transferred back to the ward. Initially you may feel some discomfort where the VNS has been put inside their body. The nurses will monitor this and give you pain relief.
If you have a good recovery, they can go home the day after the operation. Stitches are usually dissolvable and so will not need taking out.
If pain relief is still needed this can be given to take home. There may be some swelling around the device this should settle as you recover and return to normal activities.
Side Effects
Common side effects of VNS therapy are:
- Hoarseness or changes in voice tone
- Prickling feeling in the skin
- Shortness of breath
- Sore throat
- Coughing
These side effects may occur during stimulation and improve over time. If the side effects are bothersome, consultants can adjust the stimulation to lessen the side effects.
Should you continue with epilepsy medication?
It is important to follow your neurology team’s advice on what medicines to use after surgery. Even though you have the VNS, the neurology team may ask you to continue giving medication, as VNS is not a replacement for medicine. VNS is an additional treatment.
Are there any problems that can happen?
As with all operations and medical devices there is a risk of infection. If this happens you will need treatment.
The device has a battery built into it however over time this will become less efficient and will need replacing. How much the device is used will determine when the battery needs to be replaced. Battery replacement is done by the same team, in a similar operation, however only the medical device needs to be changed and not the wires.
